Battle isn’t over

County health and medical personnel believe the best way to avoid the coronavirus is to follow CDC mask protocol and get vaccinated. HEALTH FIRST
Medical, safety communities ramp up response as coronavirus cases rise
On June 19, the staff of Parrish Medical Center was anticipating a zero COVID-19 patient party in its near future. On that day, only two patients at the Titusville hospital were hospitalized with the virus.
The party, unfortunately, was not to be, because just 10 days later, Parrish was treating 46 COVID patients, six of them in the ICU.
“It was almost twice as [what we had] in July 2020,” said Edwin Loftin, Parrish’s senior vice president of Integrated and Acute Care Services and chief nursing officer.
Of the 130 patients hospitalized in the beginning of August at Parrish Medical Center, 63 were COVID-positive and 19 were on ventilators requiring ICU-level care.
As hospitals, private practices and group homes were just starting to think the worst was behind them, a major uptick, caused primarily by a younger, unvaccinated population, brought everyone back to battle mode. The three major hospital systems worked in tandem to meet the significant insurgence in cases that have nearly doubled every week for several weeks in a row.
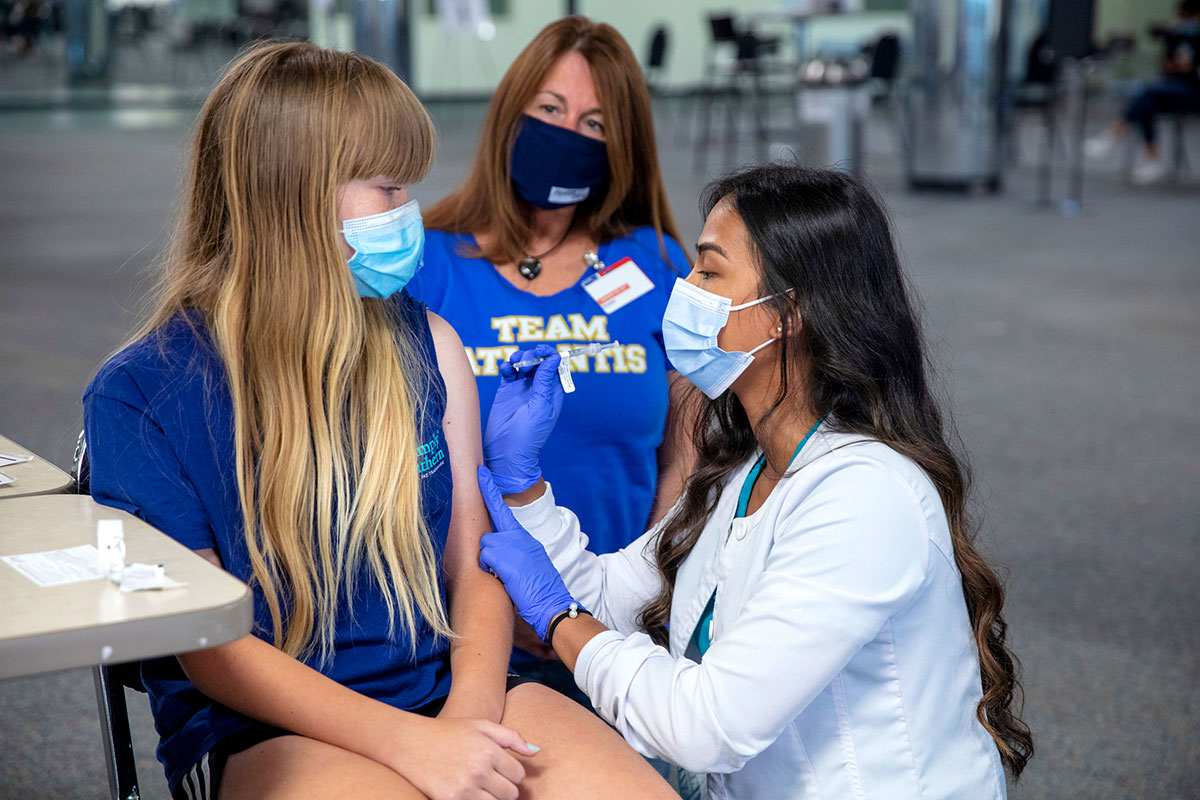
A Health First team member administers the COVID-19 vaccine to a young patient. HEALTH FIRST
OVERFLOW TENT RETURNS
In early August, Parrish activated its overflow tent in the parking lot in an effort to decompress high Emergency Department volumes and provide a safe place to treat lower acuity, non-COVID patients.
“The current surge of COVID patients is stressing every health-care system and hospital to their limits,” said Parrish Medical Center president/CEO George Mikitarian.
Drivers who went by a Health First hospital also noticed tents outside the four hospitals in the health-care system. Like Parrish’s, the tents allowed for Emergency Department overflow to treat new patients safely and open additional capacity options.
Outpatient labs at Holmes Regional Medical Center, Cape Canaveral and Palm Bay hospitals and Health First’s Diagnostic Center at Viera Medical Plaza have been working under reduced hours and services. Health First Diagnostic Center in Melbourne temporarily closed, and patients were encouraged to visit the Health First Medical Group locations for routine tests.

Health First cardiologist Dr. Khalid Sheikh discusses treatment options with a patient. Masks have been required at all Health First facilities since the start of the pandemic, and the protocol will be in place until the danger of contracting the virus subsides. HEALTH FIRST
STAFFING SHORTAGES
Patients planning elective surgeries will have to cool their heels for some time. Parrish and Health First decided to postpone scheduled non-emergency surgeries by early August to redirect resources, primarily staffing, to emergency departments, ICU and inpatient care units.
Space may have been at a premium, but it wasn’t the biggest issue.
“It’s more of a staffing issue than a bed issue,” said Health First chief physician executive Dr. Jeffrey Stalnaker during a July 30 news conference.“We’re able to flex beds for critical care patients.”
Brevard hospital staffing reflects a national trend of staffing shortages due to pandemic burnout. For a year, the nurses and other health-care workers have put in the extra shifts, the extended hours, and they are exhausted. Some opt for per diem positions.
“People are tired,” Stalnaker said.
Masks remain mandatory at hospitals. The policy requires all visitors to wear face masks, regardless of their vaccination status.
At the beginning of the pandemic, personal protective equipment, or PPE, was in short supply, but that is not the case this time around.
“At Parrish, our goal early on was to have 365 days of PPE supply, so we’re well prepared,” said Loftin.
VISITING LIMITED

Dr. Nik Moradi, medical director of Critical Care and Pulmonology at Melbourne Regional Medical Center, believes the pandemic crisis will continue for some time. STEWARD MEDICAL GROUP
At the end of July, Parrish reinstituted its no-visitor policy. Health First followed in early August. Visitors were not allowed inside except in certain situations such as labor and postpartum patients, hospice patients and pediatric patients. However, video visitations are available on request.
Like Parrish and Health First, the three Steward hospitals in the area — Melbourne Regional Medical Center, Rockledge Regional Medical Center and Sebastian River Medical Center — have all experienced déjà vu with COVID-19.
“There’s been an increase in volume across all three facilities,” said Dr. Nik Moradi, medical director of Critical Care and Pulmonology at Melbourne Regional Medical Center. “Our admission rates are way up and we project it to continue for some while.”
Moradi noted that among the patients admitted with COVID-19 symptoms, 98-99 percent were unvaccinated.
Unlike Parrish and Health First, the Steward hospitals didn’t postpone elective procedures. In fact, expanded hours allowed for previously canceled procedures to be scheduled as quickly as possible. However, a strict visitor and masking policy was in effect and ERs were reorganized for the safety of patients. The system continued to encourage alternative methods of electronic communication via Skype, etc., between patients and loved ones.
COUNTY UPDATES
The county’s Emergency Management office implemented weekly Facebook Live updates beginning early in August. During the pandemic’s first peak, the Department of Health and Brevard County Emergency Management hosted a weekly panel of county officials, including those in public safety and public schools, to provide updates on COVID-19 issues facing the community.
The return of these updates should help keep the public informed regarding what the medical community and county government are doing in response, as well as testing and vaccination locations and updated CDC recommendations. During these weekly events, the public can pose questions to the panel of experts.
By mid-August, all three local hospital systems were over capacity and continued to deal with a strong surge in patients.
According to John Scott, Brevard County emergency director, hospital emergency rooms are also seeing surges in patients with COVID-19 symptoms, though not all of those visiting the ER have an emergency situation, a situation that poses safety concerns for real emergencies such as traffic accident-related trauma patients, cardiac victims or others needing emergency treatment.
County health and emergency services officials issued a plea to consider other options before taxing ambulance services with nonemergency calls and not to show up at the ER for a COVID test when other test sites are available. Scott said people looking to be tested should do so at an urgent care, pharmacy or through their personal physicians.
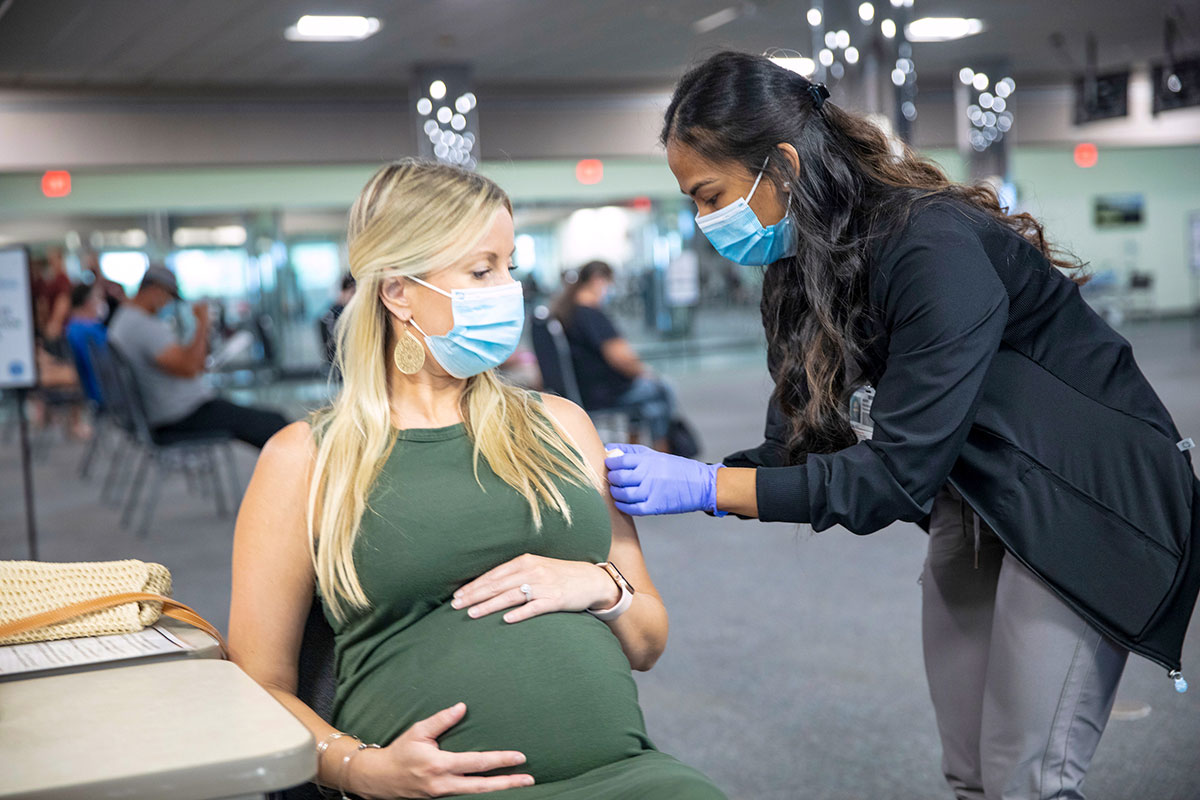
Pregnant women are encouraged to get a vaccination because of increased risk. HEALTH FIRST
TESTING DELAYS
Unfortunately, delays were being encountered where testing is available. At some locations, appointments were necessary. Others have seen long lines or are requesting patients to wait in their vehicles until notified to come inside for a test.
“[Testing] is still widely available in our community, but like anything, as the numbers go up, so too does the demand for testing,” Scott said. “The demand is up.”
Brevard County Fire Rescue Chief Mark Schollmeyer noted that its ambulance personnel were transporting approximately a dozen individuals with COVID-related symptoms per day to local hospitals, a number that equals the height of the pandemic in 2020.
The good news among all the bleak is that while hospitalizations were up, death rates were down.
“We have better treatments,” Modari said. “We’re in a better place to handle the surge.”
As more people realize the critical need for vaccination and for practicing vigilant hygiene, the surge will recede, and, perhaps those zero patient parties will finally be held. For now, Dr. Barry Inman with the Florida Department of Health in Brevard has a simple message of advice.
“The best thing to do is get vaccinated,” he said.

Maria Sonnenberg
Maria is a prolific writer and proofer for Space Coast Living and an adjunct professor at Florida Institute of Technology’s Nathan M. Bisk College of Business. When not writing, teaching or traveling, she can be found waging a one-woman war against her lawn and futilely attempting to maintain order among the chaos of a pack of extremely clueless wirehair dachshunds and an angst-driven basset hound.



