So many of the beautiful things that make living in Central Florida feel like paradise – the warm sun, theme park attractions and easy access to beaches and waterways, for example – also pose hidden (and avoidable) dangers that could have serious health consequences. With summer quickly approaching (and 300 or more days of sunshine annually here), many of us engage in a wide array of outdoor activities that have dermatologists working overtime treating pre-malignant and malignant tumors caused, in large part, by excessive, chronic sun exposure and blistering sunburns.

The most common of these skin cancers are actinic keratoses (precancerous lesions), basal cell carcinomas and squamous cell carcinomas. Basal cell and squamous cell carcinomas are cancers of the cells in the epidermis (the top layer of the skin) from which they originate. Basal cells and squamous cells make up 10% and 85% of the epidermis, respectively. Repeated sun exposure over decades eventually damages and alters the DNA of the skin cells, leading to the development of skin cancer. (Patients are typically confused and frustrated about the delayed diagnosis of these cancers, which can take as long as 30 to 40 years to develop.)
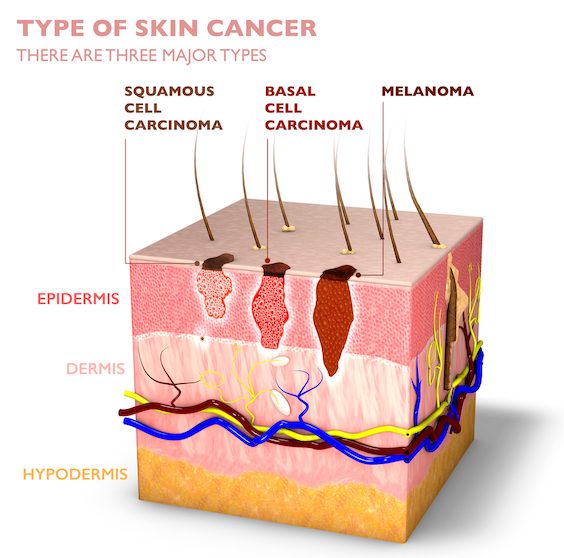
Fortunately, basal cell and squamous cell carcinomas are usually not fatal and only rarely metastasize (migrate) to other parts of the body. They are readily treated in the clinic by a wide range of surgical and non-surgical interventions.
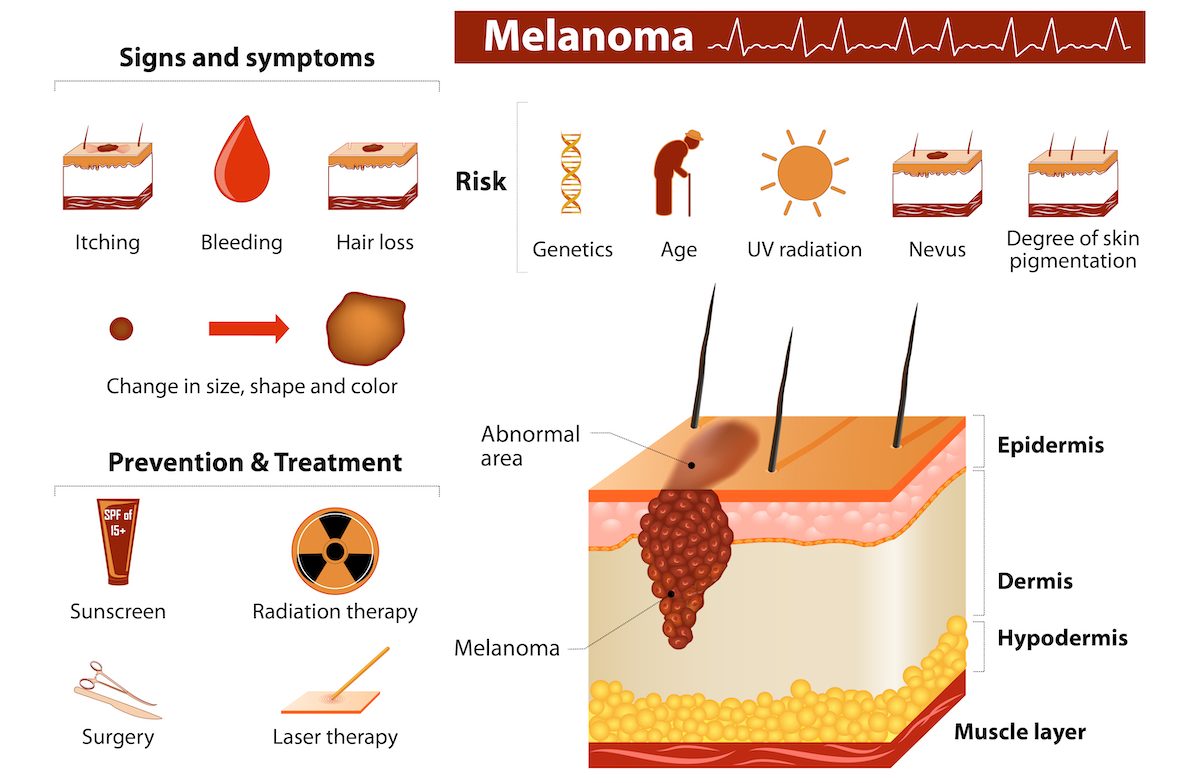
The deadliest and most challenging skin cancers to treat are malignant melanomas. Melanomas are cancers that develop in melanocytes, or the skin cells that produce melanin. Melanin is the pigment that gives your skin color. Melanomas can also occur in your eyes and internal organs.
Recent projections from the American Cancer Society estimate that nearly 100,000 new cases of melanoma will be diagnosed this year with an estimated 6,800 deaths. Melanoma can occur at any age, but it is most common in patients older than 60 and is one of the leading causes of cancer in women ages 25 to 30.
Although the exact cause of melanoma is unknown, people with fair skin have the greatest risk: white patients are 20 times more likely to develop melanoma than African American ones. However, melanomas diagnosed in African Americans, Hispanics and other ethnicities with darker skin types are typically far more advanced. This is most usually due to a delayed diagnosis as many patients with dark skin falsely believe that they will not get skin cancer.
In addition to the common risk factors of blistering sunburns and excessive sun exposure, other risk factors for developing melanoma include family history, suppressed immune system (especially among organ transplant recipients), multiple atypical moles, and prior history of melanoma. And unlike basal cell and squamous cell carcinomas, melanomas can develop in patients who have not had excessive sun exposure.
The typical melanoma appears as a brown, black and/or red irregularly shaped lesion which may be flat or raised above the skin. Other symptoms such as bleeding, itching, and pain and discomfort may or may not be present. This typical appearance accounts for the vast majority of melanomas.
However, there is another unusual clinical presentation which is seldom addressed: amelanotic melanoma. Amelanotic means “without melanin,” or without pigment. These melanomas present as red, pink or scar-like, dome-shaped lesions with little or no pigment. Due to the scarcity of color, they are typically ignored and as a result, diagnosed at a later stage. Any lesion that recurs next to a previously treated melanoma should be examined immediately, even if the lesion looks like a scar. To keep things in perspective, amelanotic melanomas account for only about 5 percent of all melanomas. They are treated by the same aggressive surgical and medical interventions that are used for the pigmented variants.
Treatment for melanomas is based on five stages (stage 0,1,2,3 and 4) of the cancer, as established by the American Joint Committee on Cancer (AJCC). The depth of the lesion is a major component of its stage. If the cancer is confined to the top layer of the skin at the time of diagnosis, it is called melanoma in-situ, and is classified at stage 0. Surgical excision, followed by routine surveillance skin exams every 3-6 months, is the recommended treatment for melanoma in-situ.
If the melanoma invades deeper than the epidermis at the time of diagnosis, the depth is measured and assigned a number. This measurement is called the Breslow depth and it plays a critical role in the behavior of the cancer. If the Breslow depth is at least one millimeter thick, the recommendation is to biopsy the sentinel (first) lymph node that drains from the site of the melanoma. The result of the lymph node biopsy plays another crucial role in the staging and subsequent treatment of the cancer.
The AJCC system uses Breslow depth, lymph node biopsy result, and other prognostic factors to establish the stage of the cancer. In the past decade, a myriad of immunotherapies for melanomas has emerged that have increased life expectancy for patients with advanced, metastatic melanoma. These therapies enhance the patient’s own immune system to help fight the melanoma.
One innovative technology – developed by the company DermTech – uses genomics to enhance the accuracy of melanoma diagnosis and avoid unnecessary biopsies of benign lesions. The technology works by rubbing an adhesive strip across the suspect lesion which harvests the RNA of the skin cell. This genomic material is sent to a lab that evaluates the tissue for specific genetic signals that are uniquely present in melanomas. This genetic material provides information that cannot be obtained through routine pathology and, If the results show genetic signals suspicious for melanoma, the lesion can be surgically removed. I have used this technology numerous times over the past several months; it’s new and exciting and helps patients avoid unnecessary biopsies.
Protect Your Skin, Save Your Life
To combat the damaging effects of too much sun exposure, we should all arm ourselves with wide brim hats, sun protective clothing, sunglasses and sunblock.
The American Academy of Dermatology recommends everyone use sunscreen that offers the following:
- Broad-spectrum protection (protects against UVA and UVB rays)
- SPF 30 or higher
- Water resistance

Additionally, planning outdoor activities before 11 am and/or after 4 pm also can help minimize ultraviolet radiation exposure.
If you notice any changes to your skin, or notice any enlarging, non-healing lesion – regardless of color – seek the immediate attention of a dermatologist. The best chances for successful treatment include early detection, prompt removal of the lesion, and continued routine surveillance.
Amelanotic melanoma is a type of skin cancer. Unlike most forms of melanoma, a person with amelanotic melanoma will develop a mole or similar growth that does not contain melanin. Melanin is the pigment that gives skin cells and moles their color.

Dr. Anthony Porter
Anthony Porter, M.D., F.A.A.D., received his medical degree and completed a formal dermatology residency at the Medical University of South Carolina. With offices in Melbourne and Suntree, Dr. Porter is board certified in dermatology and has practiced in Melbourne since 2006. For more information, call (321) 308-0659 or visit online at www.porterderm.com.



